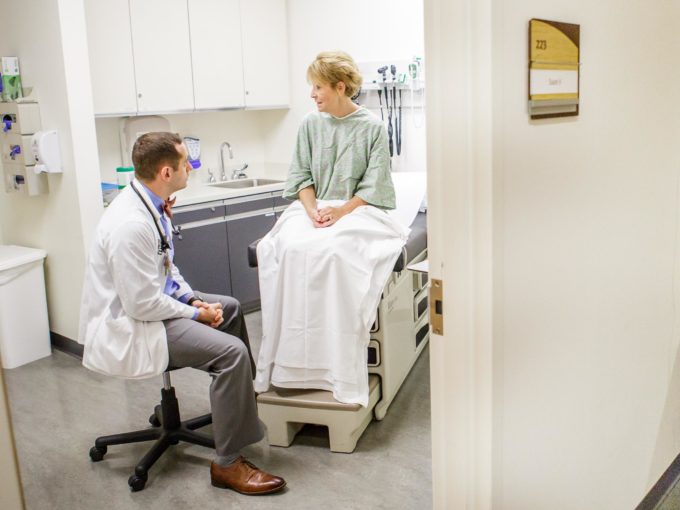
Each paragraph of this narrative is inspired by a separate patient story from my last three months of neurosurgery rotations. Each paragraph ends with something I learned to be grateful for in that challenging situation. All identifiers have been removed or changed. Some of this material may be triggering regarding death and hardship.
2:14 pm. “Why don’t you just get on out of here for the day, good job this week.” Taken slightly off-guard, I packed up my bag and said thank you to the four temporary coworkers that put up with my ineptitude for the past two weeks. On paper, it was a great day: Two cups of coffee before we ran the list, rounds that finished before 11 am, Chick-fil-a for lunch, and leaving early? Honestly maybe one of the better days of third year. I rode the escalator in silence and stepped outside to what was a beautiful day in mid-May. I paused for a moment in the outdated brick hallway, turned around, and thought to myself, “well, [expletive].”
During my Internal Medicine rotation, I cared for a Latinx patient with end stage renal disease. He had made all the recommended lifestyle changes and was taking his medication as prescribed, but was at the point in his disease progression where he most likely needed a kidney transplant. When I asked about his ongoing medical treatment, he became tearful, confiding that he was unable to get dialysis three times a week. Due to his undocumented status, he was only eligible to receive dialysis emergently when he became very ill. This health inequity broke my heart, and I decided I wanted to work on a project that would help the Latinx community in South Carolina. Jessica Accardi (M2), my partner in this project, had experiences at the Greenville Free Medical Clinic, EMT shifts, and examining health disparities through her Masters in Community Engaged Medicine, that lead her to this research project with PASOs Greenville.
Continue Reading →Two Poems
The Other Room
“They’re doing compressions!” I heard ring through the hall.
I was with a frail, elderly, demented woman though.
She’d fallen, hit her head, and had a lac that you would’ve sworn stretched from her frontal bone to her occipital.
In reality, it was less than the circumference of a dime.
The blood seemed endless, covering her scalp, completely, the way flowers cover valleys or the way snow caps mountains.
I wasn’t present with her I was curious about what was happening down the hall, in the other room.
Death. We say the word and instantly shudder. It is something our subconscious has decided to suppress from our mind. We constantly fight death – outsmarting it with medications and treatments. We study endless pathways and algorithms about death and read about it in our books. Death is looked at as a third party, something completely objective: a statistic, a number, a word on a page…until it is seen almost every day. I haven’t thought about death and dying more in my life than in the past month and a half. I know I still have a lot to learn about it, and not just in books or journal articles.
Continue Reading →Recently, I have had thought-provoking discussions with fellow classmates about being introverted. Some physicians advise students to “become more extroverted,” which is easier said than done. During these discussions, I have been consistently reminded of a piece of advice that I received during EMT training. I was told that doctors must enter a patient encounter commanding the room and demanding attention. That is not “me,” I thought. How am I supposed to do that? These thoughts led me down a winding road of self-doubt. Since those personality traits did not match my own, I found myself wondering if I would be a good physician.
Continue Reading →We are all in medical school because of other people; not one of us made it here without relying on a support system. My family was my first support: encouraging me from a young age in academics, athletics, art and music, and inadvertently teaching me never to quit or give up. More objectively, they provided me with the resources I needed to succeed, such as five years of higher education and medical school preparatory materials. My friends were my second support: they believed in me when I didn’t, and they had absolutely no doubt I was going to get into medical school.
Continue Reading →Last week, many of my classmates were posting “last day of school” photos as we completed our final classes of medical school, often captioning them something along the lines of “look you guys, I’m a doctor now!” This sent me into a reflective reverie, questioning when do I really become a doctor? Is it the last class of medical school or, more officially, on graduation day? Is it the first day of intern year, when I plunge into a patient’s room and utter the phrase “I’m Dr. Bailes, and I’m going to be taking care of you today”? Or is it some moment later when I take charge in a crisis, such as running my first code or doing a crash intubation?
I don’t have an answer to this central question. I am trying to soak in the warm salutations of my friends and family as I wait for it to feel real.
Continue Reading →Yesterday I ran. I stepped outside into the blue sky and I fled, needing to feel my lungs burn. There were daffodils dancing and children cackling as they rode their bikes. No one told the weather here the world is crying. My neighborhood all dressed up in its Easter best has no idea what’s on the horizon. It makes it all the more difficult to understand and picture that we are currently experiencing a global pandemic.
I think this palpable dissonance surrounding me perfectly reflects the tension and confusion I am feeling in this moment. I have chosen a career in medicine because I want to care for others, fix their problems, heal their pain. In a few short months I will be stepping onto the front lines of this battle against our new viral invader as an Emergency Medicine resident.
Continue Reading →These past few months have been an unprecedented time of social and economic upheaval. For many of us, the effects of the pandemic have been wide-reaching, pervasive, and personal. What began as flurry of reports from far-away places has arrived on our shores in force: an invisible enemy made material through the suffering it has inflicted, and will continue to inflict. Some, at first, looked optimistically at the case-history of similar pandemic viral outbreaks in recent memory, finding solace in their scope. While lethal, these cases relatively numbered in the few, not the many. While they did burn, and burn brightly, their candles were snuffed out. This is different. The woodshed has ignited, and the tinder is dry.
Continue Reading →